Summit targets post-op pandemic
Health & Medical
Australian health leaders are holding a national summit in Adelaide this week as data reveals a hidden pandemic in patients suffering post-surgery complications.

Sign up to receive notifications about new stories in this category.
Thank you for subscribing to story notifications.

Organiser and Royal Adelaide Hospital Professor of Anaesthesia Guy Ludbrook hopes the findings trigger a radical shakeup in post-operative care that will save more lives, reduce hospital stays and ultimately save valuable health dollars.
“We are now getting together people responsible for major health decisions to see if we can develop a major strategic plan for the problem, I think ultimately, we need a new system of care,” Prof Ludbrook said.
Prof Ludbrook co-wrote a paper for the journal Anaesthesia and Intensive Care with Dr Richard Walsh saying changes must be made or the risk of complications after surgery will increase at around 10 per cent annually over the next 30 years.
The rise is driven by the ageing population along with more chronic illness like diabetes, obesity, heart disease, and kidney disease.
Prof Ludbrook estimated that if complications after surgery in Australia fell by 15 per cent it could save the nation $1.2 billion a year, and a recent trial using a new postoperative care model showed dramatic, positive results.
This trial led by Prof Ludbrook and colleagues from three national hospitals following moderate risk patients after operations revealed a startling number of patients experienced complications in the 24 hours after treatment.
“These are not complicated cases so we would not normally think patients would get into trouble, but what we’ve discovered is that they often develop medical issues which means they would need a medical emergency team call,” Prof Ludbrook said.
Most common complications involved low blood pressure, breathing or pain problems, Prof Ludbrook, who is Director of PARC Clinical Research at the Royal Adelaide Hospital and the University of Adelaide, said.
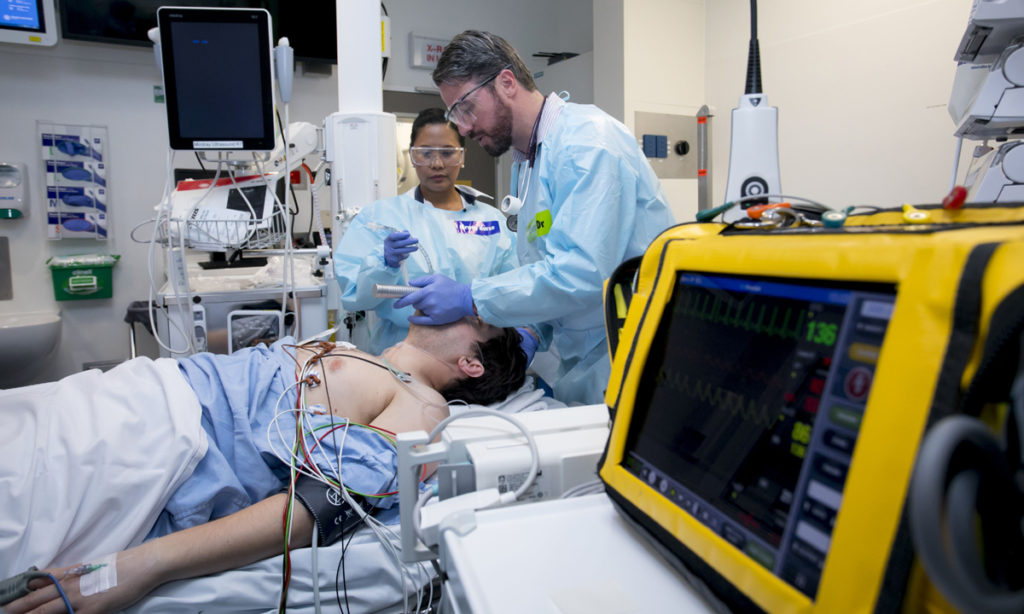
By using an advanced recovery room care (ARRC) model where patients were monitored by anaesthetists and high-level nursing staff after undergoing surgery it meant these complications were treated quickly.
The trial showed those patients then spent three more days at home in the three months after surgery.
“We have done internal cost analysis here where the estimated return on investment is around $2.50 for every $1 spent, hospitals will have to put more resources in but improvements gained more than pay for themselves,” Prof Ludbrook said.
The March 6 summit being held at the South Australian Medical Health and Research Institute is called The Hidden Pandemic of Post Operative Complications.
It draws together 80 clinicians, private and public hospital leaders, health insurers, government representatives and also two of the most senior anaesthetists in the United Kingdom, Professor Monty Mythen and Professor Mike Grocott.
Prof Ludbrook said it was vital to get the conversation started because if hospitals introduced new care models there was potential to help with emergency admissions and in freeing up beds.
“For example, the existing footprint of the Royal Adelaide Hospital is well placed to do such a thing and we estimate with 90 per cent confidence we would save about 4000 bed days a year in this hospital, freeing up about 20 beds a day,” Prof Ludbrook said.
The trial was held across the Royal Adelaide Hospital, Peter MacCallum Cancer Centre in Melbourne and Lismore Base Hospital in New South Wales.
Jump to next article




